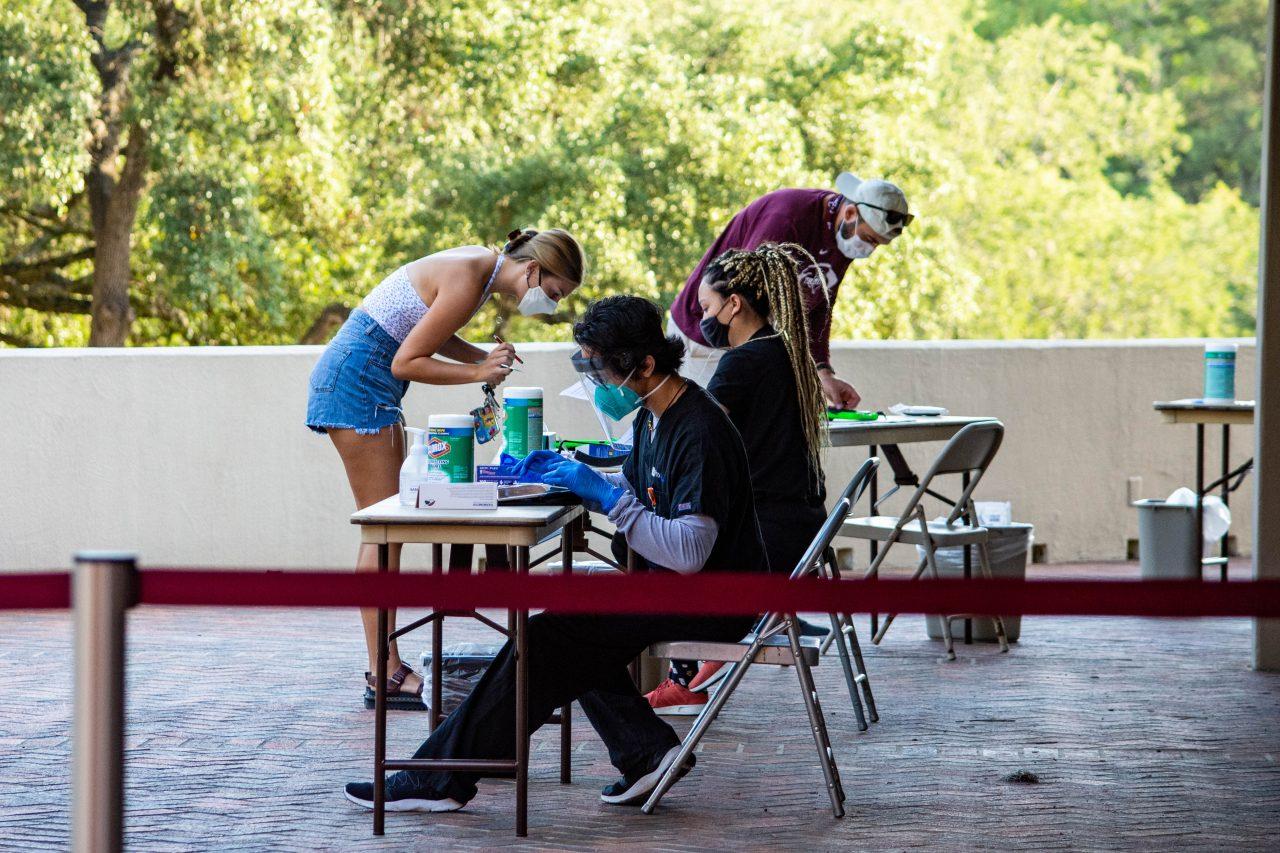Photo by Genevieve Humphreys
Face masks, social distancing, and daily health checks: While unfamiliar and wearisome at times, such precautions are necessary to preserve a semblance of normalcy in the midst of COVID-19. As part of these measures, Trinity’s administrative leaders and healthcare workers have organized quarantine and isolation procedures in the event that students are exposed to or test positive for the virus.
With an array of new COVID-19 terminology having entered everyone’s vocabulary, Tess Coody-Anders, vice president for Strategic Communications and Marketing, explains the differences between quarantine and isolation.
“Isolation is what happens when someone has tested positive for or been clinically diagnosed with COVID. Quarantine is if you had an exposure to someone who is positive, but you have not yet tested positive, so we put you in quarantine just to be safe,” said Coody-Anders.
Once a student enters isolation they are treated as highly infectious and the university begins monitoring symptoms, conducting vital signs checks, and contact tracing. The differentiation between isolation and quarantine requires a defining of “close contact,” which according to Marcy Youngdahl, university physician, is set in terms of duration and proximity of contact.
“[Close contact] is when you have been unmasked with someone for a period of fifteen minutes or longer at a distance of less than six feet. We see that the six-feet rule helps cut down on the ability of those respiratory droplets to make it to another person,” said Youngdahl. “Of course the mask comes into play because that mask is actually what’s called ‘source control,’ so it prevents some of those respiratory droplets from coming out. So, if you are unmasked with somebody, then that of course puts you at higher risk.”
Coody-Anders also emphasized the importance of wearing a mask, especially when around other students on upper-campus
“Even if you are in a study room in the library or CSI by yourself, somebody could come in right behind you so it is really important that you have been wearing that mask. If we wear our masks, give each other some space and wash our hands frequently, we can really slow this down,” said Coody-Anders.
Coody-Anders went on to note that the ProtecTU Health Check app is another important resource in controlling the spread of the virus on campus
“It’s a really great thing, that Daily Health check tool, so I would use that every day. Not only are you required to, but it is a good thing to do. Answer the questions honestly because it will help you capture any symptoms that you might be having that you may not have associated with COVID, but better safe than sorry,” said Coody-Anders.
According to Lauren Rice, junior chemistry major who is on-campus every weekday for a lab, although the app is not perfect, it does serve as an important tool to assess one’s health.
“I use it more like an affirmation that me going to campus is okay for today. It’s definitely not foolproof, there are issues with it. People could just lie and say that they are fine when they are not. But I use it as an affirmation, so I would hope that everyone else uses it that way but I am not sure,” said Rice.
If a student were to begin experiencing symptoms, Youngdahl stresses that they should reach out to the COVID-19 Health Clinic as soon as possible
“We do recommend that if you have symptoms you should get a test. For on-campus students or students that are coming to campus from the community, we recommend calling the COVID clinic. If you are off campus, you can still use the COVID clinic as a resource to see if you need to be tested,” said Youngdahl. “We do hope that people are discovering these symptoms when they are doing their morning symptom check.”
Contact-tracing plays a vital role in assessing the presence of the virus on-campus, particularly after a student begins to show symptoms. However, student confidentiality and safety are maintained throughout the contact-tracing process.
“The first thing you should do is isolate yourself and contact the COVID clinic. The second thing you should do is start to think back to the last 3-5 days. Start thinking through, ‘Where have I been? Who have I been with? What activities have I been involved in?’,” said Coody-Anders. “Check your calendar, check your social media. It is really important at that point to think about all the people who may have had exposure to the virus with you so that when the contact-tracing team calls you, you are able to help them reach out to those people as quickly as possible. It is all anonymous, so when a member of the contact-tracing team contacts you they will ask you questions about who you have been with, but when they follow up with those people they will not say who is positive.”
While she stresses that one should be tested if exposed to the virus, Youngdahl notes that a negative test result will not shorten one’s quarantine due to COVID-19’s long infectious period.
“There’s an infectious period, and we keep people in quarantine for 14 days from their last exposure because during those 14 days you could develop symptoms or become infected with the virus. It is a misconception for a lot of people of, ‘Why do I have to stay in quarantine if you can just test me and know that I don’t have it?’ But it’s not simple,” said Youngdahl. “You could miss a period of time where the virus is at a high-enough amount to show a positive result.”
Students in isolation are offered a wide array of resources including clinical support, academic aid and mental health consultations, all overseen by Emma Phearse, case manager and care navigator.
“All of the quarantining and isolating students have what is called a care navigator, an individual who reaches out to them to make sure they understand exactly what is going to happen to them while they are in quarantine or isolation. The care navigator makes sure that the student knows exactly what to expect, and they coordinate getting food, laundry, trash, pick-up, all that for the students,” said Coody-Anders. “Then they get a call from Emma Phearse, who is our new case manager at Trinity, who works with them to determine, ‘Would like some time with counseling services? Do they need some extra academic support? Do they need help contacting their professors to talk through options and alternatives?’ She works with them on that. And lastly, the clinical team checks in on them every day.”
Coody-Anders noted that the care team is equipped with the resources needed to care for a variety of students and unique needs.
“We had some students early on, so they needed to have books that just came in to the bookstore picked up and delivered. Or, we had one student where it was his birthday while he was in quarantine, so his parents wanted to send him something and the catering services picked up that item for him and put together a birthday spread and took it to his room. And we had an athlete who got his normal meals for the day but was still super hungry and needed a special meal, so the care navigator made sure that the student got whatever extra they needed. It is pretty intensive, and that’s why we say there is a capacity level on what we can handle without leaving students to their own devices,” said Coody-Anders.